Limit to Scholarly / Peer Reviewed American Indian Homelessness
- Research
- Open Admission
- Published:
Experience of healthcare amongst the homeless and vulnerably housed a qualitative study: opportunities for equity-oriented health care
International Journal for Equity in Health volume 18, Commodity number:101 (2019) Cite this article
Abstract
Groundwork
People experiencing homelessness are ofttimes marginalized and are known to face barriers to accessing adequate and respectful healthcare services. This study examines the experience of accessing hospital-based services of persons experiencing homelessness or vulnerable housing in southeastern Ontario and considers the potential of Equity-Oriented Health Intendance (EOHC) as an approach to improving intendance.
Methods
Focus groups and in-depth interviews with people with lived experience of homelessness (n=31), too as in-depth interviews of health and social service provider key informants (n=x) were combined with qualitative data from a survey of health and social service providers (n=136). Interview transcripts and written survey responses were analyzed using directed content assay to examine experiences of people with lived experience of homelessness inside the healthcare arrangement.
Results
Healthcare services were experienced as stigmatizing and shaming particularly for patients with concurrent substance use. These negative experiences could lead to avoidance or abandonment of care. Despite supposed universality, participants felt that the healthcare system was not accountable to them or to other disinterestedness-seeking populations. Participants identified a system that was inflexible, designed for a perceived eye-class population, and that failed to take into account the needs and realities of equity-seeking groups. Finally, participants did identify positive healthcare interactions, highlighting the importance of care delivered with dignity, trust, and pity.
Conclusions
The experiences of healthcare services among the homeless and vulnerably housed do not meet the standards of universally attainable patient-centered care. EOHC could provide a framework for changes to the healthcare system, creating a system that is more trauma-informed, equity-enhancing, and attainable to people experiencing homelessness, thus limiting identified barriers and negative experiences of care.
Groundwork
This study explores the experience of hospital-based healthcare for people who are vulnerably housed or homeless. Literature suggests that the healthcare system is either inaccessible to or fails to run across the needs of certain groups. Data outlines barriers to intendance for Indigenous Canadians, members of the LGTBQ* community, persons experiencing ongoing or historical trauma, persons using substances, and those experiencing homelessness or who are vulnerably housed [1,2,3,4,5,half dozen,7,8,ix,10]. Thirty-five thousand Canadians are homeless on whatsoever given night and 235,000 Canadians experience homelessness in a year [xi]. Average life expectancy for homeless persons is estimated at betwixt 42 and 52 years [12, xiii]. Betwixt 44 and 60% of people who experience homelessness will apply illicit substances in their lifetime [11, 14, fifteen].
The primary objective of the Canada Health Deed, the foundational legislation of Canada's universal healthcare system, is "to protect, promote and restore the concrete and mental well-being of residents of Canada and to facilitate reasonable access to health services without fiscal or other barriers" [16]. This would imply that health services must be tailored to eliminate avoidable barriers to admission, and should actively seek to protect, promote and restore the health of all Canadians, including the most marginalized.
Data in this study derives from a mixed-methods study funded by the Due south East Local Health Integration Network (SELHIN) (Ontario, Canada) exploring palliative intendance services for the homeless and vulnerably housed. In this study, "homelessness" or "vulnerably housed" includes those who are living out-of-doors, in substandard weather condition not fit for human habitation, in temporary or unstable accommodations, in shelters, and those who are at run a risk of losing their existing housing [17].
Methods
Written report design
A survey was used to obtain information from health and social services providers (HSSPs) and interviews were conducted with key informants (KIs) from this grouping. A survey forth with focus groups and in-depth interviews collected data from participants with lived feel of homelessness. See Fig. 1 for an outline of all data collection and Boosted file 1 for survey tools and interview guides. Ethics approval was obtained through Queen'south University Health Sciences and Affiliated Educational activity Hospitals Research Ethics Lath.
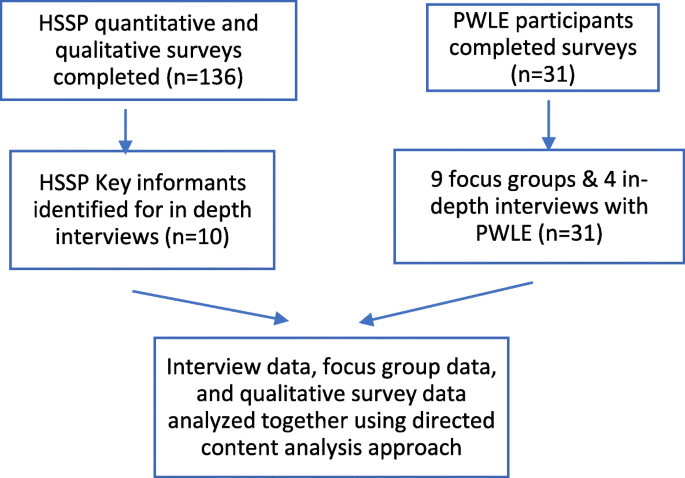
Data drove
Participants and sampling.
Health and social service providers (HSSPs)
A survey was distributed by e-mail widely to organizations throughout the SELHIN who piece of work with people experiencing homelessness (mental health and addiction agencies, housing agencies, legal aid, shelters, food programs, community health centres, primary and palliative intendance providers among others). The survey included questions about the participant's organization, scope of exercise, and thoughts and opinions on the provision of care to people experiencing homelessness with an explicit emphasis on end of life care. All questions were multiple choice, however they all had free text spaces in which participants could include comments and other considerations. 136 HSSPs responded to the survey.
Following survey collection, community agencies identified KIs who had been employed by the arrangement for at least 1 twelvemonth and had provided front end line services (past or current). KIs were a mix of urban, rural and semi-rural. Research administration conducted ten in-person or telephone interviews using a semi-structured interview guide exploring themes that were developed following review of the survey findings: challenges in accessing palliative care services by people experiencing homelessness; the impact of substance use on service acceptability and admission; education and resources required to back up people experiencing homelessness and/or substance employ; and recommendations for organization changes. Interviews lasted approximately 60 min and were conducted by research assistants or by the principle investigator (MM).
Persons with lived experience (PWLE)
Persons with experience of homelessness were recruited from agencies mandated to provide services to those who are vulnerably housed. Snowball sampling was used to recruit further participants. Inclusion criteria was a by or nowadays history of homelessness. Participants completed a survey collecting bones demographic variables, information on education, housing, service use, self-rated mental and physical health, and substance use. Support was provided when literacy was a business organisation. Six focus groups were held with two to vii participants, forth with iv in-depth interviews, all lead by inquiry assistants or by the principle investigator, virtually of whom had feel working with people with lived experience of poverty and substance apply. The intent was to run focus groups exclusively, but due to scheduling challenges, several participants were interviewed individually. Both interviews and focus groups used the same semi-structured interview guide exploring themes related to how homelessness affects access to palliative intendance, the touch on of substance use, thoughts on decease and dying, and recommendations to ameliorate cease of life intendance for vulnerably house people. Theme saturation was reached prior to the end of the information collection menstruum in that no new themes were appearing in the interviews and focus groups, notwithstanding due to the importance of including the community in the research process, the want to have a big number of participants with lived experience, and the fact that other participants had already been recruited and expected to participate, 2 terminal focus groups were completed. 31 people participated, the sessions lasted betwixt 2 and iii h and were held at Street Health Centre in Kingston. Participants were given a stipend of l$ for their participation.
Data Analysis.
KI interviews and focus groups were audio-recorded and transcribed. HSSP surveys free text responses provided sufficiently rich written content to include with the transcripts. While initially reviewed for findings relevant to palliative care, transcripts were reviewed a second time by both researchers seeking themes related to access to and experience of healthcare services in general. Transcripts and survey responses were reviewed, analyzed and coded every bit one information set by 2 independent researchers, both of whom have experience with vulnerable populations as well as research and clinical experience in trauma and violence informed and EOHC approaches. Themes were then reviewed collaboratively by the 2 researchers to ensure consensus. The analysis was informed by directed content analysis [xviii, xix] which can be used when there is existing theory about a miracle, but this theory is incomplete. It is notable that for the PWLE, very few had had outset-hand personal feel with finish of life care, and much of their discussion related to the provision and receipt of healthcare services more than broadly. Data was sufficiently rich that at that place were extensive findings related to healthcare experiences in general, and that theme saturation was felt to be reached for these themes despite this not having been the original focus of the projection.
Results
Quantitative information volition be reported in particular elsewhere [20, 21]. Sociodemographic information relevant to the discussion is included in Table 1.
Qualitative findings
Participants' experience of either accessing services themselves, or of assisting clients to admission services, was predominantly negative. Four themes were highlighted by participants: (i) experiences and consequences of stigma and shame when accessing healthcare; (ii) lack of accountability of the healthcare system towards equity seeking populations; (3) inflexibility of the healthcare arrangement; and (4) positive experiences that warrant give-and-take for what they teach usa about potential improvements.
Experience of stigma and shame when interfacing with the healthcare system
The experiences of stigma among PWLE were overwhelming. In some cases, the stigma was and so painful that it superseded any wellness complaints, previous trauma, or other concerns a patient might have. Stigma was by far most pronounced in the context of current or documented history of substance employ, fifty-fifty if substance was remote, compounding the sense of shame and stereotyping.
Box 1 Participant Quote
I'll share a story that was shared with me. [This woman] had suffered a brutal rape. Horrific. Absolutely horrific. She was a woman in her belatedly 40s. Lived on the street throughout her whole life, back and forth. She was telling me her story. She needed to share it […] and she didn't cry. Not one tear when she talked about the abuse that she endured [..]. She wept when she talked most how she got treated at the hospital because she was bleeding then profusely and she flinched at a needle and the comment from the nurse was made to her: 'Well expect at your arms, every bit if you have a problem with needles". That weighed so heavily and this is when the woman broke downward. The abuse was horrific but she had almost been marinating in that level of violence and corruption all her life. The devastating role of information technology all was the shame she felt from the hospital […] because of her I.5. drug use. (KI iv).
Stigma, or predictable stigma, had important consequences for health. Every bit reported by others [22], PWLE avert care due to by negative experiences. They might exit in the centre of a care session, fifty-fifty removing intravenous lines in order to extricate themselves from intolerably stigmatizing situations. PWLE were often isolated from back up networks when in care because their support networks, coming from the same social contexts, were equally stigmatized and occasionally overtly excluded by healthcare providers. PWLE lacked trust towards healthcare providers due to by experiences which had significant impacts on their care seeking behavior and likelihood of post-obit through on provider recommendations. Finally, PWLE and HSSPs had many examples in which they felt that complaints were not taken seriously, oftentimes due to a history of substance utilise, which caused them to fear that they would be unable to obtain appropriate care.
Box 2 Participant Quote
It really got and then bad that I actually unhooked my IV and left the hospital and didn't get back. […] I just couldn't. believe it. It was scary actually considering when I unhooked that Iv, I thought to myself: 'What am I doing here?' That's how scared I was that they really set information technology off in me that I started to think 'Oh god, now they are going to do this to me and now they're not gonna take proper intendance of me.' (FG1A).
The presence of an advocate from outside of their social network (eg. a social services worker or pastoral care worker), had a significant impact on the care patients received. While this was more than probable to enable them to receive care in a respectful and appropriate way, it farther highlighted the stigma they experienced when their advocate was not present.
Lack of accountability of the healthcare system towards equity-seeking populations
Participants felt that the healthcare system was not answerable to the people it served. Participants articulated the responsibility of healthcare providers to provide fantabulous, empathic intendance to everyone who presents, regardless of their socioeconomic status, substance use history, or life circumstances. Healthcare providers were felt to take a lack of understanding of the bear upon of social determinants of health, ongoing trauma and past adversity on people's health and healthcare presentations. Examples were given of clients asked to leave the hospital because of the way they dressed or smelled. Participants felt that healthcare providers lacked knowledge around impairment reduction, around the root causes of substance use and arduousness, and that they appeared to lack empathic or compassionate curiosity towards patients and the difficulties they encountered.
Box 3 Participant Quotes
"Being homeless- I hateful people look at you every bit though y'all're a low life, piece of crap. I hateful, you're a drug addict and everything else. You're not worth the shit that you sleep in [..]. You're restricted because of the way y'all look. Y'all're on the street. You don't have a place. Doors are shut. People just shun yous and everything else" (FG9B).
"You know it's all those kids we think near when we hear these horrific news stories of corruption. They went into the foster intendance arrangement and and so we don't think of them again just that trivial kid ends up being the thirty-year-old. with a criminal record and that little kid ends upwardly being a woman who's prostituted for the last 10 years." (KI4).
Respondents wanted to come across medical practitioners whose priority were their patients rather than status, job security, or finances. They also felt that having peers with lived feel of substance use, homelessness, or other disinterestedness-related challenges operating within the healthcare system would help make care more accountable and acceptable for them and others.
Box 4 Participant Quote
"If you're going to bring new [healthcare providers] in, then you educate them to be this way and if you. don't treat this way. […] I mean - there's a proffer box [..]! You lot're going to stand up answerable. Allow'south get the government accountable. Allow'south get everybody accountable who'south looking after the states. I AM a human beingness. If you're not gonna to treat me like a homo being - well you're going to hear it correct from me." (FG1B).
Inflexibility of the organisation
HSSPs described a healthcare organisation that was not tailored to meet the needs of their clients. The organization was described every bit designed past eye class people for middle class clients, expecting conformity to the organization rather than tailoring the arrangement to the differing needs, desires and challenges of patients. Examples included the requirement that housing be obtained before handling could be initiated when housing was not an option; a lack of flexibility for patients who might bear witness up late or miss appointments; and a lack of openness to a harm reduction approach that might permit patients to receive a tailored class of handling in the context of substance utilise rather than being dismissed out of mitt.
Positive experiences
While the majority of the discussion, both from HSSPs and PWLE, focused on negative experiences of intendance, in that location were also some positive encounters related to healthcare experiences where providers upheld nobility, autonomy and choice for patients, where they provided flexible, non-judgemental services in spaces where clients felt welcomed. Participants used terms such as "trust" and "compassionate" to describe these positive experiences of care.
Box 5 Participant Quotes
"She's a nurse here aye. I admire her. I adore her. I respect her and I trust her and she's the sweetest girl that. I've ever had – the sweetest medical care person I've ever had have intendance of me. She'due south merely amazing […] Yep.
similar she's very very thorough and she's very compassionate. I merely, oh my heart'southward with her, I beloved her. Yeah."
(FG9BRM1)
"They are really like, hey we similar the temper of this identify. We similar that people hither care for u.s. really squeamish and we're people. We experience loved. There are paramedics here who are, you know, assisting us. Um we really experience rubber in this space and like there's no judgement and we want to keep coming dorsum hither." (KI9).
Discussion
Our findings echo the negative experiences and resulting impacts on health and healthcare access of equity seeking populations described in other studies, including the homeless and vulnerably housed [1,2,3,4,five,six,7,viii, 10, 23]. These include intendance avoidance, stigma, inflexibility of the current system, unmet healthcare needs and a lack of harm reduction philosophies integrated into the delivery of care.
While listening to the voices of our participants is key to understanding the inadequacies of our system, listening to these voices also presents an opportunity for alter. There is pocket-sized and increasing trunk of literature on Disinterestedness-Oriented Wellness Care (EOHC) and trauma and violence informed care in healthcare settings simply these theories are rarely applied to hospital-based medicine and do not accost hospital-based medicine for the homeless or vulnerably housed. We believe that the articulation of EOHC [24,25,26] as an approach may present united states with a road map and tools to answer to the concerns of homeless and vulnerably housed clients, particularly with respect to their concerns well-nigh discrimination, stigma, and inflexibility of the organisation every bit articulated in our study and others [23, 27].
EOHC rests on three components. The first is trauma and violence informed care (TVIC) that recognizes the prevalence of past and ongoing trauma in people's lives and acknowledges the way in which trauma affects people's physical and emotional wellness, interpersonal relationships, and ability to access care. TVIC rests on five principles [28]: [1] Trauma sensation and acknowledgement; [2] Rubber and trustworthiness; [3] Choice, control and collaboration; [4] Strengths based and skills edifice; and [five] Cultural, historical, and gender issues. The principles of TVIC are echoed in participants' narratives. Participants shared the corking burden of past and ongoing trauma that people facing homelessness and substance use have experienced. The need for safety and trust were explicitly articulated, as well as the challenges in developing that trust. Choice, command and collaboration are the antithesis of the stigmatizing and dismissive care that participants too oftentimes received in healthcare encounters, which is neither strengths based nor skills building. Finally, much literature supports the ongoing impact of gender, ethnicity, indigeneity and history on access to care [four, vi, eight].
The 2d component of EOHC is damage reduction. About of the literature examining PWLE of homelessness place substance employ and the healthcare system'due south response to substance utilise, as significant concerns [ii, fourteen, fifteen, 23]. Harm reduction encompasses programs, practices, policies and philosophies that aim to reduce the harms of substance use, viewing substance utilize as a health outcome rather than a moral failure [26]. Participants feel that healthcare providers view their substance use as making them less worthy of dignified care and less valuable every bit human beings. A harm reduction approach requires a central shift in how the healthcare arrangement interacts with people who use substances. In add-on to formal policies and programs, such an approach requires us to see the people behind the substance employ, to recognize their dignity, experiences, trajectories, and challenges.
Cultural safety is the third component of EHOC. Culturally safe care is particularly important in the Canadian context where Indigenous people keep to experience the negative effects of electric current and by colonization [vi, 29] but would be relevant in any context of human diversity. Culturally safe care explicitly addresses inequitable power relations, racism, discrimination, and furnishings of historical and current inequities within health intendance encounters [29]. More than just an attitude, culturally safe care requires knowledge of history and of the root causes and consequences of inequity on the part of healthcare providers.
Finally, EOHC requires that an arroyo to and delivery of care be developed with input from all stakeholders, including people with lived experience, just also all members of the healthcare squad from physicians and nurses to janitors and receptionists. A recent study has found that cantankerous sector collaboration that provides integrated health intendance improved barriers to access and also enabled cocky-managed care [30]. These changes crave leaders to engage non simply with providers who are already advocates for equity-seeking populations, but also with those who are non. EOHC presents a unique opportunity to build partnerships amidst professional person and patient groups that rarely mix outside of clinical intendance and allows a system to be responsive to the local needs of its population. Communities with higher rates of substance use, higher percentages of Ethnic clients, or recent loss of employment with increase in precarious housing could meet the challenges and opportunities presented past EOHC differently.
Limitations
The HSSPs in our report were most all involved in providing intendance to homeless and vulnerably housed individuals and were more often than not self-described advocates for this group. Our study might have benefitted from integrating the voices of HSSPs who are non specifically committed to working with equity-seeking populations. Additionally, our data was originally collected in the context of work on palliative care. Further questions specifically targeting other healthcare experiences might accept yielded boosted data. Nevertheless, our findings are amply supported by the extensive verbal and written discussions around healthcare services from all study participants and align with findings in the literature as well [1,ii,3, ten, 23].
Conclusions
There are ii cardinal messages in our findings: The first is that the intendance nosotros are providing to our most vulnerable clients is not adequate and does non run into the professional standards of accessibility, universality, and patient-centeredness. An ofttimes-quoted line by Dr. Edward Trudeau from the 1800s proposes that the dr.'southward role is "to cure sometimes, to relieve frequently, to comfort ever". Our findings demonstrate that for sure groups nosotros may be declining on all three counts.
Our second bulletin is that we believe there is a style to raise our healthcare organisation to this standard, and that EOHC, developed locally and tailored to place, provides a route map from where we tin can begin. EOHC requires a cultural shift within our profession, away from the standardized one-size-fits-all care we have get used to and back, perhaps, to a more versatile, artistic way of delivering care that many of us aspire to. It volition crave team work in hospitals and clinics, changes to curriculum in medical and nursing schools and continuing professional development. Information technology will crave those who promise to exist leaders in this field to have compassion and understanding for colleagues for whom this is more difficult. Finally, it will require us to not merely heed to, merely to hear and to see the patients before us in all their forcefulness, complication and occasional despair, to consider the trajectory and meaning of their lives within our broader lodge, likewise equally our own privileged place therein.
Availability of information and materials
All transcripts of interviews and focus groups, survey responses, and quantitative data are bachelor from the authors upon request. Quantitative data is currently nether consideration for publication elsewhere.
Abbreviations
- EOHC:
-
Equity-Oriented Wellness Care
- HSSP:
-
Health and social service provider
- KI:
-
Key information
- SELHIN:
-
S Due east Local Health Integration Network
- TVIC:
-
Trauma and Violence-Informed Intendance
References
-
Grech East, Raeburn T. Experiences of hospitalised homeless adults and their wellness care providers in OECD nations: a literature review. Collegian. 2019;26(i):204–eleven.
-
Martins DC. Experiences of homeless people in the wellness care delivery system: a descriptive phenomenological study. Public Health Nurs. 2008;25(5):420–30.
-
Skosireva A, O'Campo P, Zerger Southward, Chambers C, Gapka Southward, Stergiopoulos Five. Different faces of bigotry: perceived discrimination among homeless adults with mental disease in healthcare settings. BMC Health Serv Res. 2014;14(1):376.
-
Chisolm-Straker M, Jardine L, Bennouna C, Morency-Brassard N, Coy L, Olivia Egemba M, et al. Transgender and gender nonconforming in Emergency departments: a qualitative report of patient Experiences2017. p. 8–16.
-
Dubin RE, Kaplan A, Graves L, Ng VK. Acknowledging stigma: its presence in patient intendance and medical education. Can Fam Doc. 2017;63(12):906–viii.
-
Wylie L, McConkey S. Insiders' insight: discrimination confronting indigenous peoples through the eyes of Health Care professionals. J Racial Ethn Health Disparities. 2019;6(ane):37–45.
-
van Boekel LC, Brouwers EP, van Weeghel J, Garretsen HF. Stigma among wellness professionals towards patients with substance utilize disorders and its consequences for healthcare delivery: systematic review. Drug Alcohol Depen. 2013;131(1–2):23–35.
-
Bauer GR, Scheim AI, Deutsch MB, Massarella C. Reported emergency department abstention, use, and experiences of transgender persons in Ontario, Canada: results from a respondent-driven sampling survey. Ann Emerg Med. 2014;63(6):713–xx e1.
-
Felitti V, et al. Adverse childhood experiences (ACE) questionnaire. 1998. Available at: https://www.ncjfcj.org/sites/default/files/Finding%20Your%20ACE%20Score.pdf. Terminal Accessed xx June 2019.
-
Argintaru N, Chambers C, Gogosis East, Farrell S, Palepu A, Klodawsky F, et al. A cross-sectional observational study of unmet wellness needs among homeless and vulnerably housed adults in three Canadian. cities. 2013;13(one):577.
-
Roy East, Boudreau JF, Leclerc P, Boivin JF, Godin G. Trends in injection drug use behaviors over 10 years among street youth. Drug Alcohol Depen. 2007;89(2–3):170–5.
-
Stephen Gaetz ED, Richter T, Redman M. The state of homelessness in Canada 2016. Toronto: Canadian Observatory on Homelessness Press; 2016.
-
Huynh L, Henry B, Dosani N. Minding the gap: access to palliative care and the homeless. BMC Palliat Intendance. 2015;14:62.
-
G-YM MNR. Illicit drug use as a challenge to the delivery of end-of-life care services to homeless persons: perceptions of health and social services professionals. Palliat Med. 2012;26:350–nine.
-
Grinman MN, Chiu S, Redelmeier DA, Levinson Westward, Buss A, Tolomiczenko K, et al. Drug problems among homeless individuals in Toronto, Canada: prevalence, drugs of option, and relation to health status. BMC Public Health. 2010;10. https://bmcpublichealth.biomedcentral.com/articles/10.1186/1471-2458-10-94.
-
Government of Canada. Canada Health Act. Available at: https://world wide web.canada.ca/en/health-canada/services/health-care-organisation/canada-health-care-system-medicare/canada-health-act.html. Last Accessed xx June 2019
-
Gaetz S, Barr C, Friesen A, Harris B, Hill C, Kovacs-Burns Grand, Pauly B, Pearce B, Turner A, Marsolais A. Canadian Definition of Homelessness. Toronto: Canadian Observatory on Homelessness Press; 2012.
-
Pope CZS, Mays North. Qualitative enquiry in healthcare: analysing qualitative data. Br Med J. 2000;320:114–6.
-
Assarroudi A, Nabavi FH, Armat MR, Ebadi A, Vaismoradi M. Directed qualitative content analysis: the description and elaboration of its underpinning methods and information analysis procedure. J Res Nurs. 2018;23(1):42–55.
-
Purkey EM. M. Experiences of death, dying, and accessing the palliative healthcare system for homeless and vulnerably housed individuals and their suggestions for system redesign. J Am Board Fam Med. 2019. in printing.
-
MacKenzie MP. Eastward. Health and social services providers feel, power, and comfort level in providing cease of life services to persons experiencing homelessness. Journal of the American board of family unit medicine. J Am Board Fam Med. 2019. in printing.
-
Hudson BF, Flemming K, Shulman C, Candy B. Challenges to access and provision of palliative care for people who are homeless: a systematic review of qualitative research. BMC Palliative Care. 2016;15. https://bmcpalliatcare.biomedcentral.com/manufactures/10.1186/s12904-016-0168-half-dozen.
-
Campbell DJ, O'Neill BG, Gibson Yard, Thurston We. Primary healthcare needs and barriers to care amid Calgary's homeless populations. BMC Fam Pract. 2015;16:139.
-
EQUIP Health Care. What is Wellness disinterestedness: a tool for Health & Social Service Organizations and providers. Vancouver BC; 2017.
-
EQUIP Wellness Care. Cardinal dimensions of equity-oriented Intendance: ten strategies to guide organizations in enhancing capacity for equity-oriented Health Care.; 2017.
-
EQUIP Healthcare. Promoting Health disinterestedness - damage reduction 2018. Available from: https://equiphealthcare.ca/equip/wp-content/uploads/2018/04/HRT-Apr-17-2018.pdf. [cited 2018 October 25]
-
Shulman C, Hudson BF, Depression J, Hewett N, Daley J, Kennedy P, et al. End-of-life treat homeless people: a qualitative analysis exploring the challenges to admission and provision of palliative care. Palliat Med. 2018;32(one):36–45.
-
Purkey East, Patel R, Phillips SP. Trauma-informed care: better care for everyone. Tin can Fam Doctor. 2018;64(three):170–two.
-
EQUIP Emergency. Promoting Wellness Equity for Ethnic and Non-Ethnic People in Emergency Departments in Canada: Projection Summary. 2018.
-
Parsell C, ten Accept C, Denton M, Walter Z. Cocky-management of health care: multimethod study of using integrated wellness care and supportive housing to address systematic barriers for people experiencing homelessness %J. Aust Health Rev. 2018;42(3):303–viii.
Acknowledgements
The authors would like to thank the inquiry assistants (Megan Singh, Agniesczka Fecica, Travis Mitchell, Amanda Brierly, Regan Lavoie), Dr. Alex Leung for written report pattern feedback. Lastly, thanks to the participants who agreed to share their deeply personal and oft difficult stories to shape our agreement.
Funding
Funding for this projection was received past the Southward East Local Health Integration Network (SELHIN) in Ontario, Canada.
Author information
Affiliations
Contributions
MM was the principle investigator for this report. She conceptualized the study, developed the inquiry tools, and coordinated the survey, focus groups and interviews. She reviewed and coded the qualitative and survey data, and contributed to the drafting and editing of the manuscript. EP was the co-investigator. She provided consultation during the research process, reviewed and coded the qualitative and survey data, and led the writing of the manuscript. Both authors read and approved the terminal manuscript.
Corresponding writer
Ideals declarations
Ideals approval and consent to participate
Ethics approval was obtained through Queen'south University Health Sciences and Affiliated Teaching Hospitals Research Ethics Board.
Consent for publication
Non applicable.
Competing interests
The authors declare that they accept no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Additional file
Additional file ane:
Appendix A. Health Care and Service Providers Survey. Appendix B. Participant with lived feel Survey. Appendix C. PWLE focus group and interview guide. Appendix D. KI Interview guide. (DOCX 26 kb)
Rights and permissions
Open up Access This article is distributed nether the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted employ, distribution, and reproduction in whatever medium, provided you requite appropriate credit to the original writer(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Artistic Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data fabricated available in this article, unless otherwise stated.
Reprints and Permissions
Virtually this article
Cite this article
Purkey, Eastward., MacKenzie, Grand. Experience of healthcare among the homeless and vulnerably housed a qualitative study: opportunities for equity-oriented health care. Int J Equity Health 18, 101 (2019). https://doi.org/10.1186/s12939-019-1004-4
-
Received:
-
Accustomed:
-
Published:
-
DOI : https://doi.org/ten.1186/s12939-019-1004-iv
Keywords
- Homelessness
- Wellness equity
- Vulnerable populations
Source: https://equityhealthj.biomedcentral.com/articles/10.1186/s12939-019-1004-4
Post a Comment for "Limit to Scholarly / Peer Reviewed American Indian Homelessness"